When you look at the current state of America’s massive nationwide coronavirus testing network, two things stand out.
The first is that it is a logistical marvel. Four months ago, the COVID pandemic caught many of our leaders completely flat-footed and unprepared; today, most anyone in America can make an appointment at a nearby clinic or pop-up testing station, with or without a doctor’s referral, get a nose or throat swab within a few hours, and have results in hand in a matter of days. After months of largely reactive testing, we’ve taken major steps to ramp up proactive testing too: among hospital patients, nursing home residents, the imprisoned. Our labs churn through more than 600,000 tests every day; some days that number is closer to a million. It’s a staggering feat.
The second thing is that it’s not sufficient—at least not compared with the major bump in recent infections the country is currently experiencing. So far this month, the U.S. is setting daily records for new COVID cases. While testing is not yet as overwhelmed as we were back in the spring—part of the reason we’re seeing so many new cases is because testing has grown so robust—the evidence is beginning to mount that our testing apparatus is creaking beneath the strain.
Two main metrics are relevant here. First, there’s the test positivity rate, which tracks what percentage of COVID tests come back positive and thus helps us gauge the strength of our testing apparatus relative to the strength of the virus. Second, there’s the test turnaround time, which gives a sense of how backlogged the labs processing the tests are getting. Turnaround time is also important when it comes to assessing how effective tests are in general: When it comes to influencing people’s behavior, it’s far more useful for them to know whether or not they have coronavirus within a day of taking the test than within a week.
By both metrics, the outlook is worsening. According to the disease watchers at Johns Hopkins and the COVID Tracking Project, the test positivity rate steadily decreased between late April and early June, as mass social distancing helped slow the virus down enough for testing to catch up. According to this metric, we were at our best during the first two weeks of June, during which time the test positivity rate hovered around 5 percent—only one positive case out of every 20 tests run. Since then, however, the rate has been ticking up steadily: Wednesday’s results landed above 8 percent. (It’s worth remembering too that this information, as with all information related to the spread of the virus, comes to us on a delay.)
Meanwhile, the two enormous testing centers responsible for processing most of America’s COVID tests, LabCorp and Quest Diagnostics, have both announced in recent days that patients should brace for longer wait times as they struggle to meet the latest spike in demand.
“In recent weeks, we have seen a steady increase in demand for molecular testing and we are doing everything we can to continue delivering results in a timely manner while continually increasing testing capacity,”: a LabCorp spokesperson told The Dispatch. “With the recent increase in demand, results on average may take 1-2 days longer.”
A spokesperson for Quest Diagnostics told The Dispatch the company has had to slow turnaround times by a few days as well.
“It is fair to say our turnaround time is on par with what it was in late March and early April,” she said. “However, it is important to note that during this time we were performing about 25,000 to 30,000 tests per day. Now we’re at 115,000per day, so that should give some perspective on how dramatic the increases in volume are, but also how far we’ve come from a capacity perspective.”
Long turnaround times for tests were troubling back in March and April, but they’re potentially even more damaging today. In the spring, with nearly every state enforcing some kind of lockdown and almost everyone already practicing social distancing religiously, a positive COVID test didn’t have as much bearing on individual human behavior. Now that many Americans have started to inch back toward regular life, however, a COVID test has become an extremely disruptive event, generally requiring a dive back into isolation pending the results. Longer waits can mean more lost income, lost weeks of life, and can even discourage people who think they may have been exposed to the virus but are not showing symptoms themselves from getting tested at all.
And all that’s just the nationwide picture. In the nation’s worst viral hotspots the testing situation is starting to approach meltdown status. In Florida, the test positivity rate is now 19 percent. In Arizona, it’s a staggering 27 percent.
In some places, problems are even starting to crop up at the point of testing. Spiking cases in testing have led to not just turnaround delays, but actual testing shortages of the kind not seen since the pandemic’s early days. Several cities in Texas, including Austin, have begun to reinstate limits on who is eligible to receive a test. Asymptomatic people are being turned away. City officials in Houston and Dallas say that their public testing sites are running through their day’s allotment of kits most days by around noon.
In other words, our testing apparatus is operating least effectively in precisely the places it’s most desperately needed. All of this makes tracking the virus that much more difficult and continued state reopenings that much more dangerous.
It’s worth noting in discussing these things that some of this backsliding is unavoidable. We are, after all, still engaged in fighting the first battle against a virus that remains very new and about which we still know far too little.
Nevertheless, this sort of streaky test coverage can be blamed at least in part on a federal COVID response that seems more absent than ever. After spending months closely monitoring the federal effort against the “invisible enemy,” President Trump has plainly moved on, focusing instead on the national reopening, shreds of economic good news, and his presidential campaign against Joe Biden. When he does address the pandemic these days, it’s mostly to kvetch that the media is blowing the virus out of proportion once again or to quarrel with the assessments of his own top experts.
Not that it’s hard to see why, when those experts are back to striking a much more dire tone than the president wants to hear. “There are parts of the United States, like [New York], that are doing really well, that you’ve been through something really bad and you have things under control,” Dr. Anthony Fauci, the nation’s top epidemiologist, told FiveThirtyEight on Thursday. “But as a country, when you compare us to other countries, I don’t think you can say we’re doing great. I mean, we’re just not.”
Taken altogether, it paints a grim picture. We’ve weathered one wave of horrific disease and death, and seem well on our way to a second. Whatever unity of public purpose helped us get through April and May seems to have evaporated. And the sandbags we’ve been able to place against the renewed onslaught of the virus are weakening as a result.
“You have to be having blindfolds on and covering your ears to think that we don’t live in a very divisive society now, from a political standpoint,” Fauci said. “I think you’d have to make the assumption that if there wasn’t such divisiveness, that we would have a more coordinated approach.”
“We don’t have a national plan. We don’t have a national strategy,” former FDA commissioner Scott Gottlieb, a leading expert on the coronavirus pandemic, told CNBC Monday. “We don’t have a national pool of resources and swing capacity that we can move around when we have these epidemics, and so states start to get pressed very quickly. … It’s a bigger problem than we thought it would be at this point.”
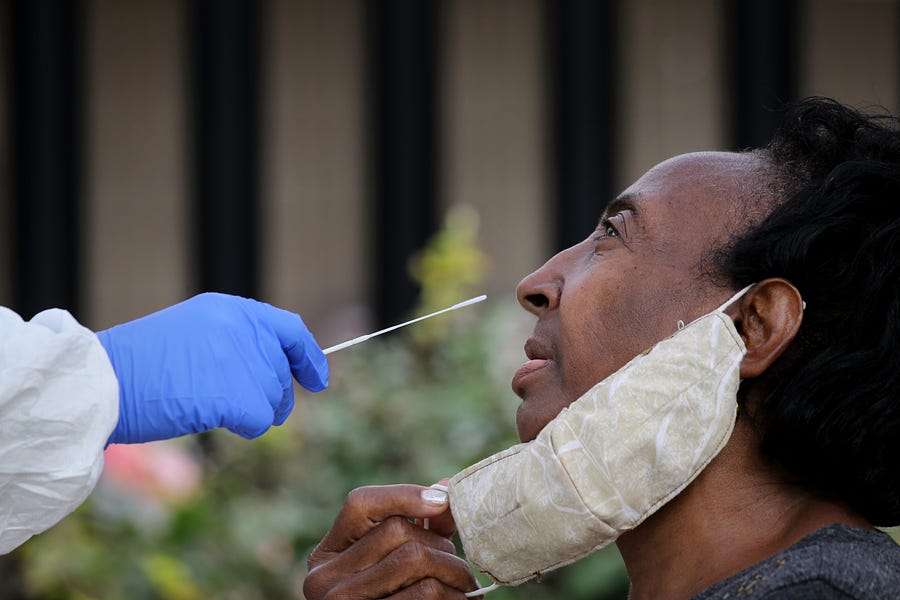
Photograph by Craig F. Walker/The Boston Globe/Getty Images





Please note that we at The Dispatch hold ourselves, our work, and our commenters to a higher standard than other places on the internet. We welcome comments that foster genuine debate or discussion—including comments critical of us or our work—but responses that include ad hominem attacks on fellow Dispatch members or are intended to stoke fear and anger may be moderated.
With your membership, you only have the ability to comment on The Morning Dispatch articles. Consider upgrading to join the conversation everywhere.